Sharon has 21+ years of experience as a qualified Emergency Care Nurse registered with the Australian Health Practitioner Regulation Agency (APHRA) and 12+ years as a First Aid Trainer.
She takes pride in FirstAidPro making first aid training available, comprehensive and affordable to everybody.
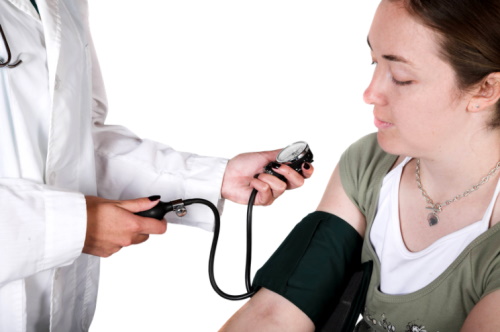
Hypotension is the fancy medical name for low blood pressure – meaning the internal pressure of the blood in your veins and arteries is lower than normal. Blood pressure can vary greatly from person to person, but if it gets low enough, it can start to show distinctive symptoms and potentially cause you some health problems.
But what causes hypotension? How critical is it, and can it ever become dangerous or life-threatening? And how do you help someone suffering the symptoms of hypotension?
For starters, let’s have a look at what hypotension is, and how it affects people.
What Is Hypotension?
The blood in your body is under pressure at all times. While this might seem like an uncomfortable idea (“What if I spring a leak??”), it’s actually a very good thing. Blood is a liquid, so it flows down to the lowest point by default. The fact your blood is under pressure means that when your heart pumps it, it goes where it’s needed – like your brain – rather than just trickling down into your feet.
Think of it a little like the water in your house. Having water pressure helps the water come up through the pipes and out your taps where it can do some good. No water pressure? No water.
The blood in your veins changes pressure constantly as your heart beats and pushes blood through the system. It’s at its highest when the heart is pushing blood through your arteries and at its lowest between heartbeats.
To measure your heartbeat, doctors usually give two numbers. These numbers are the highest and lowest pressure that the blood in your veins reaches each time the heart beats (known as the systolic pressure and diastolic pressure, respectively). This is measured in what’s called millimetres of mercury – normally written as “mmHg”. The average human blood pressure alternates between 120 mmHg and 80 mmHg – or as a doctor would say, “120 over 80”.
Normal human blood pressure varies a fair bit, so being lower than the average isn’t necessarily a big deal. But if your blood pressure is unusually low, it can mean blood doesn’t always get to where it’s needed, causing you problems. This is what we refer to as hypotension or low blood pressure. Many Doctors define the edge of hypotension as having a blood pressure of 90 over 60. If either of your numbers is that low or lower, you officially have hypotension.
Low blood pressure isn’t necessarily a critical medical issue – it’s more of a condition to be monitored. It’s generally regarded as far preferable to high blood pressure (or hypertension), which carries a considerable risk of stroke and heart failure. It’s only if your blood pressure drops extremely low that there’s any real risk.
What Is The Main Cause Of Hypotension?
That’s a very tricky question to answer. There are actually a vast number of things that can cause hypotension, so there’s not really anything you can point to as the main cause. Some of the common causes of low blood pressure include:
- Medications (including some antidepressants and heart medicines)
- Pregnancy
- Certain types of emotional stress
- Medical conditions such as heart disease, Parkinson’s, diabetes, or thyroid disease.
- Blood loss from an accident or injury (less blood means less blood pressure)
- Internal bleeding
- Anaphylactic shock
- Dehydration (which reduces blood volume)
- Donating blood
- Some allergic reactions
- Certain types of infection
- The body overheating
- Lack of nutrients in the diet
What Are The Symptoms Of Hypotension?
Hypotension can show itself in various ways, but some are more common than others. Some of the most frequent symptoms include:
- Lightheadedness or dizziness
- Feeling fatigued
- Nausea or discomfort in the stomach
- Clammy skin
- Blurry vision
- Struggling to concentrate
- Feeling like you’re going to faint
- Losing consciousness
These symptoms can occur at any time but are more likely to occur when changing position or doing something physically strenuous (like straining on the toilet). This is because with low blood pressure, such actions can alter the blood flow to the brain and other critical organs.
When Is Low Blood Pressure An Emergency?
Low blood pressure on its own is not an emergency. If you’re persistently experiencing symptoms such as faintness when standing up, it’s worth getting to a doctor soon to get checked out, but there’s no need to be calling 000 immediately.
The only time that hypotension requires immediate medical intervention is when a person’s blood pressure has dropped far enough that they’re going into shock. This means the person may not be getting sufficient blood flow to the brain. This is often due to an additional medical issue, such as blood loss from an injury or Anaphylaxis (a severe allergic reaction). The signs of shock include many of the symptoms of hypotension but may also include difficulty breathing, anxiety, confusion or disorientation, an irregular heartbeat, a dry mouth and vomiting.
If someone is showing signs of shock, then you do need to call 000 at once.
How Is Hypotension Treated?
Regular hypotension doesn’t usually require treatment as such – if you’re suffering from hypotension, you’ll need to discuss it with a doctor to see what treatment might be needed, what warning signs you need to watch out for, and what activities you might need to avoid. Any treatments they recommend will generally consider the type of hypotension you’re suffering from, the factors causing it, and your own state of health.
However, if someone near you is showing signs of shock, then medical intervention IS needed. After calling for an ambulance, you should make the person comfortable – lie them down and keep them warm. Loosen tight clothing, and if possible, elevate their feet up above their head to allow the blood from their legs to flow down into their brain. Stay with them until help arrives, and reassure them, but don’t allow them to move about or give them anything to eat and drink – even if they’re thirsty.
You should note – the above advice can provide general guidelines for treating shock, but they are not a substitute for professional first-aid training. To be adequately prepared to assist someone suffering from shock – and a wide range of other medical emergencies – there are few better ways you could invest your time than spending a day doing an accredited first aid course.