Sharon has 21+ years of experience as a qualified Emergency Care Nurse registered with the Australian Health Practitioner Regulation Agency (APHRA) and 12+ years as a First Aid Trainer.
She takes pride in FirstAidPro making first aid training available, comprehensive and affordable to everybody.
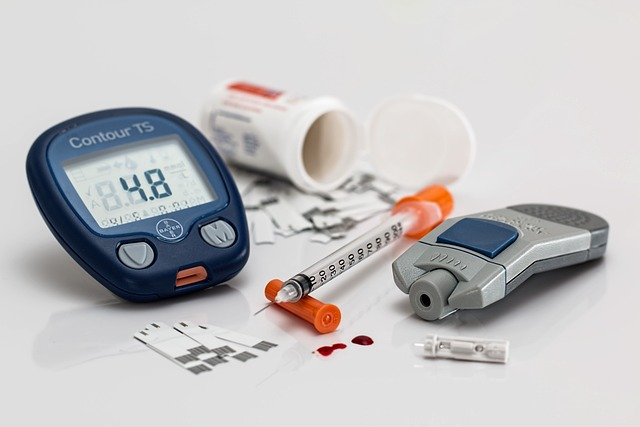
Diabetes affects how your body processes sugar, leading to high blood glucose (sugar) levels. It isn’t just a single condition but 3 distinct varieties that are complex and require round-the-clock monitoring and care.
It’s important to manage diabetic levels as short-term effects can force the kidneys to overwork while long-term heightened levels can damage blood vessels and nerves, with compounding effects on the kidneys along with bonus consequences for the heart, brain, feet and eyes.
By managing sugar levels, you reduce your risk of developing life-threatening complications and improve your overall health, which is usually accomplished through a doctor-directed combination of medication, diet and exercise.
What is Diabetes
Sometimes referred to as dextrose, blood sugar or corn syrup, glucose is a form of simple sugar (also called a monosaccharide), a subcategory of carbohydrates – think cereals like rice, wheat, potatoes and many processed foods.
Carbohydrates are one of the three macronutrients that are required to sustain life, the other 3 being fats like milk, butter or cooking oils, and proteins like meat or eggs. The body makes the glucose in these macronutrients available through the catabolic (breaking down) function of metabolism.
In the human body and biology in general, glucose is the number 1 fuel source, and its concentration in blood is primarily regulated by the insulin interaction.
Insulin is an anabolic (building up) hormone, secreted by beta cells in the pancreas in response to sensing high levels of blood sugar, speeding the uptake of glucose in the body’s cells and bringing levels back down to normal.
Diabetes is when this insulin interaction malfunctions and glucose isn’t absorbed by the body’s cells, resulting in abnormally high levels of glucose in the blood.
Type 1 Diabetes
The human body is incredible and can do amazing things, however, it can also commit baffling acts of self-sabotage as in the case of autoimmune diseases, wherein the immune system inexplicably attacks an otherwise perfectly healthy part of the body. Nearly any part of the body can be infected from the thyroid (Graves’ Disease) to the intestinal tract (Crohn’s Disease) to the beta cells in the pancreas – enter Type 1 Diabetes.
Type 1 diabetes usually starts suddenly in childhood or adolescence. The main sign is, naturally, very high blood sugar from a partial or total reduction in insulin production, which can manifest early symptoms such as:
Increased urination
Increased thirst
Weight loss which can occur over days or weeks.
Children may also have:
Increased appetite
Blurred vision
Bedwetting
Skin infections
Irritability and consequently problems at school.
Symptoms, if left untreated, can lead to Diabetic Ketoacidosis (DKA) which causes:
Dehydration
Nausea and vomiting
Rapid heartbeat
Confusion
Trouble breathing or hyperventilation
This can progress quickly to a diabetic coma and even death.
While there are risks such as genetics, certain chemicals or drugs and environmental factors, the exact cause is unknown, there is no known method of prevention and there is no cure. The good news is, like many autoimmune diseases, there is treatment.
People with type 1 diabetes need to take insulin regularly to control high blood sugar levels by injecting insulin under their skin several times a day. They need to adjust the amount of insulin they take based on what they eat, their blood sugar levels and how active they are.
The goal is to keep blood glucose levels within a normal and healthy range throughout, which is usually between 80-130 mg/dL before meals and less than 180 mg/dL after meals, which can be checked at home by pricking a finger and using a glucose meter or a continuous glucose monitor.
Type 2 Diabetes
Type 2 diabetes is the most common type and is, fortunately, preventable. Where Type 1 is a malfunction of the immune system, Type 2 is a result of diet and lifestyle factors which lead to too much sugar and an over-stimulation of the beta cells in the pancreas. Consequently, over time major organs begin to build up a resistance to insulin in a vicious cycle where the beta cells begin to overcompensate and overwork themselves to the point of hyperinsulinemia. Meanwhile, the blood glucose level remains unimpacted.
Exhausted from overstimulation, beta cell function and volume will begin to collapse like a star that burns twice as bright and now, while insulin may still be produced, its effectiveness is significantly hobbled. The liver and both adipose and muscle cells have lost their ability to respond to insulin, and glucose-lowering medications and insulin injections may be required.
Symptoms can include:
Headaches
Feeling dizzy
Leg cramps
Volatile swings in moods
Being very thirsty and hungry constantly
Going to the bathroom constantly
Feeling tired and lazy constantly
Cuts and other injuries may take a long time to heal
Itchy skin and infections
Blurry eyesight
Either gaining or losing weight slowly
Generally, Type 2 diabetes is managed with dietary and lifestyle modifications paired with medication and insulin injections.
While not possible for 100% of cases, remission may be possible for some people with diabetes, and though it isn’t a cure or a reversal it does mean that a glucose level below Type 2 diabetes levels has been achieved and eventually a reduction or even cessation of some medications is possible.
Overall the goal of treatment is avoidance of the most grave complications and the promotion of better health. A long and fulfilling life is entirely possible for all who are diagnosed with Type 2 diabetes.
Gestational diabetes
This specific type of diabetes (also called GDM) occurs only during pregnancy and can affect the health of both the parent carrying the baby and the baby itself. In Australia, it’s the fastest-growing type of diabetes, impacting between 5 and 10 per cent of people embarking upon pregnancy, sharing many overlapping risk factors with Type 2.
Risk factors unique to GDM include:
Having previously had GDM during a prior pregnancy
Having one or both of the parents being over the age of 35-55
Having previously had a Very Big Baby (weighing more than 4.5kg)
Having previously returned results indicating elevated blood glucose levels
Having Polycystic Ovary Syndrome
Having parentage of certain ethnic groups like First Australians, Pacific Islanders and South Asians
Noteworthy is the reality that despite these defined risk factors 40-60% of women with GDM lack verifiable risk factors and the vast majority who develop it exhibit no obvious symptoms, either. Pregnant people need to receive regular prenatal care in general, as many will be familiar with being told, but specifically to monitor for gestational diabetes.
Untreated GDM directly impacts birth, increasing the risk of pre-eclampsia and needing a Caesarian Section, with the greatest risk being to the child, potentially resulting in stillbirth. Long-term, the baby that survives poorly treated GDM can be at higher risk of developing Type 2 diabetes or obesity later in life.
Treatment is usually straightforward and usually comprises a change in diet and lifestyle, occasionally the adoption of some medications and, even less commonly, insulin injections.
Fortunately, GDM resolves itself after the baby’s birth 9 times out of 10 and, when adequately treated, a majority of incidences result in minimal impact on the pregnancy, birth or the health of the child.
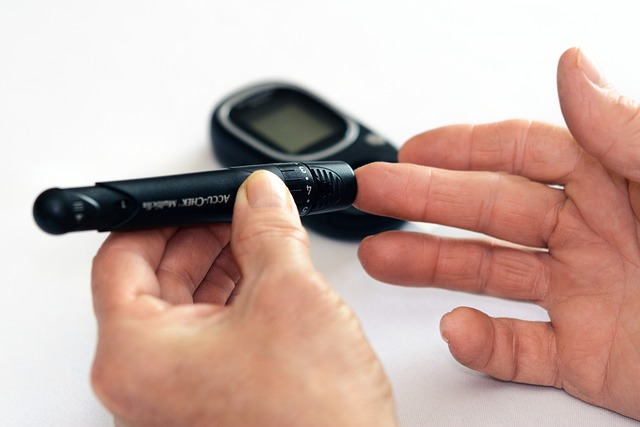
Understanding Blood Sugar Levels
Low Blood Sugar (Hypoglycemia)
When the body of a diabetic person experiences a lack of adequate blood sugar, also known as hypoglycemia, this can cause various symptoms, including:
Feeling shaky
Feeling dizzy
Feeling confused
Sweating
Headaches
Blurred vision.
High Blood Sugar (Hyperglycemia)
The opposite is an excess of blood sugar, known as hyperglycemia, and it can cause symptoms like:
Increased thirst
Frequent urination
Fatigue
Blurred vision
Diabetic Complications
Diabetic Ketoacidosis (DKA)
DKA is a short-term complication of Hypoglycemia that is often a symptom of undiagnosed Type 1 due to being a result of extremely low insulin. It can also arise in diagnosed diabetics who miss injections or have faulty pens/pumps, who have had high and prolonged stress levels or who have taken drugs or consumed alcohol.
When the body doesn’t have enough insulin, and cannot access glucose it switches instead to metabolising fatty acids, which produce acidic ketone bodies that, in the blood in large quantities, can cause severe illness that can alter the pH of the blood. Symptoms can look like:
Feeling confused and lost
Dehydration
Strange breath smell, often compared to pear drops
Heavy and difficult breathing or hyperventilating
Rapid heart rate
Vomiting and nausea
DKA is a serious condition that can quickly progress to a diabetic coma and even death, but contacting emergency services swiftly when the signs are identified can significantly improve the survival rate.
Hyperosmolar Hyperglycemic State (HHS)
HHS is a complication of Hyperglycemia that persons with Type 2 diabetes are more susceptible to, resulting from a lack of insulin. Like DKA it can also present in individuals with Type 1, however, where it differs from DKA is a lack of ketoacidosis. Symptoms can look like:
Dehydration
Feeling weak
Changes in awareness
Signs of problems with the nervous system like blurry vision, headaches, seizures, muscle jerks and even temporary paralysis
Problems with movement like weak muscles, slow reflexes, shaking or twitching
Increased thickness of blood and a higher chance of blood clots
Nausea, stomach pain and vomiting
Low blood pressure when standing up
These complications manifest slowly, lasting over a few days and taking days or even weeks to develop, during which time the individual may have also lost weight.
Due to HHS carrying the risk of progressing to diabetic coma, it should be considered an emergency and if you recognise these symptoms in someone call emergency services immediately.
Diabetic Coma
If left untreated, severe hypoglycemia, Hyperosmolar Hyperglycemic State (HHS) and Diabetic Ketoacidosis (DKA) can rapidly deteriorate into a diabetic coma.
Before a diabetic person’s condition deteriorates to the point of loss of consciousness there are signs and symptoms that you can look out for, which include:
Confusion, dizziness, feeling tired or erratic
Rapid heartbeat, profuse urination or sweating
Difficulty breathing, nausea or even seizures
If you suspect someone is experiencing a diabetic coma, call for emergency medical help immediately.

First Aid for Diabetes Emergencies
Hypoglycemia First Aid
Low Blood Sugar is not immediately life-threatening, but without treatment, a person’s condition can quickly deteriorate. Follow these first aid tips to avert further complications:
Help the person to lie down or sit in a comfortable position
To alleviate or prevent difficulty breathing, loosen any tight clothing
Give them a sugary drink or snack like fruit juice or candy – double-check it’s not a ‘diet’ or ‘no sugar’ product
Continually give them some kind of sugar every 15 minutes until they feel that they have recovered enough, then follow up with any simple and readily available carbohydrates like fruits or
If they become unresponsive or unable to swallow it is time to stop providing them with food or drinks and call for emergency medical assistance.
Hyperglycemia First Aid
If someone is experiencing extremely high blood sugar levels their life is not in immediate danger, but their condition needs to be alleviated and monitored. When hyperglycemia can get life threatening is in a remote location when you may need to offer first aid. The most immediate course of action is to try to reduce blood glucose, which can be done by:
For a diagnosed diabetic who understands their own condition and is well enough to do so you may only need to provide assistance if they request it, so be sure to ask them first if they need help first
For someone who has not been diagnosed as diabetic but who checks off many of the boxes for risk factors and symptoms they may need to seek further medical care
Ask them if they have their medication, and if they need assistance administering it
Encourage them to drink plenty of water and supply them with it if they request it
Observe their condition and be ready to contact emergency services if it worsens
Diabetic Coma
When DKA, HHS or severe hypoglycemia deteriorates the individual can be at risk of entering a diabetic coma. this can be rare because in most cases a diabetic person’s family, friends or caretakers will have identified the symptoms of the aforementioned complications before deterioration has progressed to this state.
However, diabetic comas do still happen, in which event it should be treated as an emergency because the individual’s breathing may stop and this puts them at risk of brain damage due to lack of oxygen to the brain.
Contact emergency services immediately.
While waiting for help to arrive, try to keep the person calm and comfortable by placing them in the recovery position to minimise harm.
You may be tempted to provide the person with a sugary drink or snack, but in a situation where the individual is lapsing in consciousness, they can lose control of their swallowing or coughing reflexes, making it hazardous to introduce fluids or solids to the throat. Only give a fully conscious person food or drink.
Refrain from trying to administer any insulin, as this may not correctly address the cause. Remember that diabetic coma can come from multiple complications, and you may not be aware of which.
Monitor the person’s breathing and be ready to perform CPR if the person begins to have difficulty breathing.
When emergency services arrive they will be able to assess the diabetic individual’s condition, but be ready to answer any questions they may have.
Final Thoughts
Managing diabetic levels through doctor-directed medication, diet, and exercise can help reduce the risk of complications and improve overall health for all types. However, severe complications and even diabetic coma can still occur, which is why it’s important to understand the symptoms and the basic first aid that can help mitigate further harm to the individual.
Frequently Asked Questions
How do you feel when your sugar level is low?
A low level of blood sugar may make you feel weak, shaky, dizzy, or confused. You may also feel hungry, sweaty, or have a headache. These symptoms can happen quickly and can be dangerous if not treated.
What are 5 signs your blood sugar is too low?
Low levels of blood sugar can cause various symptoms, including shakiness, sweating, dizziness, confusion, and weakness. These symptoms can occur when your blood sugar level drops below 70 milligrams per deciliter (mg/dL). If you experience any of these symptoms, you should check your blood sugar level and consume a source of glucose, such as fruit juice or candy, to raise it.
What is the best thing to eat when your blood sugar is low?
When your blood sugar is low, the best thing to eat is something that will raise it quickly. Foods that are high in carbohydrates, such as fruit, juice, or crackers, can help. It’s important to avoid foods that are high in fat or protein, as they can slow down the absorption of glucose into your bloodstream. It’s also important to eat small, frequent meals throughout the day to keep your blood sugar levels stable. If you have diabetes, it’s important to work with your healthcare provider to develop a plan for managing your blood sugar levels.
Should I eat anything if my blood sugar is high?
It’s important to know that eating can affect your blood sugar levels. If you have high blood sugar, it’s best to avoid foods high in sugar or carbohydrates. Instead, choose foods that are low in sugar and high in fibre, such as vegetables, fruits, and whole grains. It’s also important to stay hydrated by drinking plenty of water. If you’re unsure about what to eat, it’s best to consult with a healthcare professional or a registered dietitian.