Sharon has 21+ years of experience as a qualified Emergency Care Nurse registered with the Australian Health Practitioner Regulation Agency (APHRA) and 12+ years as a First Aid Trainer.
She takes pride in FirstAidPro making first aid training available, comprehensive and affordable to everybody.
A defibrillator is one of the world’s most iconic pieces of medical technology. It’s a device that can literally return the dead to life with a dramatic jolt of electrical energy, and they’re featured in countless medical dramas, action movies, and post-apocalyptic computer games. They’re also one of the most advanced pieces of medical equipment available to the general public.
But exactly how do they work? How accurately are they portrayed in movies and television, and how effective are they? Let’s take a look at this amazing medical innovation, and talk about exactly what it can (and can’t) do.
What Does A Defibrillator Do?
Defibrillators are medical devices designed to be used on someone suffering cardiac arrest. They use a powerful electrical jolt to restore the person’s normal heart function and resuscitate them.
Cardiac arrest is most commonly caused by ventricular fibrillation. That’s when the electrical activity in the heart becomes chaotic, causing the heart’s lower chambers to quiver chaotically – or “fibrillate”. This is terrible news for the victim, as it means the heart cannot effectively pump blood around the body and into the brain. And without a fresh steady supply of oxygenated blood to the brain, people are normally dead in a matter of minutes.
The common misconception about cardiac arrest is that the heart has stopped entirely, and the defibrillator “jump-starts” the heart – like someone might jump-start a car. Ironically, this is almost the opposite of what happens. In reality, the heart is still functioning – it’s just doing it wrong, meaning the blood isn’t getting pumped. As such, the job of a defibrillator is actually to stop the heart. The jolt temporarily shuts down the heart, giving the body the chance to restart with a more normal rhythm. So it’s less like jump-starting a car and more like turning a computer off and on again in the hope that it will fix the problem.
In fact, contrary to popular media, if a heart has stopped altogether (referred to by medical professionals as asystole, or “flatline”), a defibrillator can’t help. At that point, CPR and intravenous drugs (such as adrenaline) given by medical professionals are really the only hope.
How Long Have Defibrillators Been Around For?
The idea of using an electrical current to stop and restart the heart has been around a long time. It was first demonstrated at the end of the 19th century (1899 to be precise) by two swiss physiologists who found they could use small electrical shocks to cause cardiac arrest in dogs and larger ones to reverse the process. However, this wasn’t put into practice with humans until many decades later. In 1930, the first working defibrillator was built (by an electrical engineer) and also tested on dogs. It wasn’t a great time to be a dog.
Finally, in 1947, the procedure was used successfully to revive a human – a 14-year-old boy. The process took place during surgery, with the paddles being applied directly to the heart.
Then in the early 1950s, a soviet scientist in Kyrgyzstan pioneered the idea of closed-chest defibrillation – where the paddles are applied to the outside of the chest (rather than directly to the heart during surgery). After this, defibrillation became a far more practical option for resuscitation, and the ’50s saw the development (and increasing use) of various commercial brands of defibrillator.
Oddly enough, portable defibrillators didn’t see common use in Australia until the early nineties. In the ’70s and ’80s they were specialist equipment at best, and very few ambulances carried them. All this changed in 1990 when Australian media mogul Kerry Packer suffered a cardiac arrest. Purely by chance, the ambulance which responded to the call was carrying a portable defibrillator, which was used to revive him. Upon recovery, Packer donated a large sum of money to the New South Wales ambulance service on the proviso that it be used to outfit every single ambulance with a portable defibrillator unit. In memory of this, the devices are sometimes nicknamed “Packer Whackers” in Australia.
What Is An AED?
There are several different types of defibrillator available on the market nowadays. The models used in hospitals are relatively advanced pieces of medical equipment designed to provide doctors and paramedics with detailed information and allow a great deal of control about how and when to defibrillate and what voltage to use. But they’re designed for trained experts – in the hands of a layman, they could do more harm than good.
An AED is a different kind of tool altogether. The AED is a defibrillator designed to be used by members in the public. They’re easy to use, readily available, and most importantly, it’s very difficult to hurt anyone with one.
What Does AED Stand For?
AED stands for Automated External Defibrillator. Unlike manual defibrillators, AEDs are designed to do much of the work for you. Older versions came with detailed written instructions, but most modern AEDs have an automated voice that walks you through the process of assessing the state of the patient and hooking up the AED correctly.
Once an AED is hooked up to the patient, much of the work is done. It’s designed to scan their heart rate and vital signs and make its own decision about whether defibrillation is needed. Some versions have a button that you use to shock the patient (when instructed by the machine), while others even take care of that for you – detecting that a shock is required and then loudly warning people to stand clear before administering the shock.
There are two main reasons why this is important. Firstly, the device will only shock a patient when it’s needed (after warning everyone to stand clear), lessening the chances of a mistake. And second, by taking those decisions out of your hands, they take the pressure off you as the first aid provider. You’re far more likely to attempt defibrillation when you know you can’t really make a mistake.
Most ambulances, police, and emergency services now carry AEDs as standard. They’re also available in many public venues such as shopping malls and community centres as emergency medical equipment.
Who Can Use An AED?
An AED is designed to be as easy to use as humanly possible – there are no real restrictions on who can use an AED, as long as they can read and follow instructions. In an emergency, even a child might be able to use one – guided by the automated voice. And because the AED only shocks people when it’s connected up and detecting a “shockable” heart rhythm, there’s limited risk.
Of course, if the option is there, the ideal person to make use of an AED is someone who’s done proper first aid training – either a specific CPR course (which covers correct use of an AED), or any of the more comprehensive first aid training courses – almost all of which include basic CPR as a component. When someone’s suffering cardiac arrest and every moment counts, having someone who’s already familiar with using an AED can shave critical seconds off the time needed to get it working.
When To Use A Defibrillator?
The process of assessing the condition of a potential cardiac arrest victim is a well established one, generally remembered by the acronym “DRSABCD” – or “Doctors ABCD” for something a little bit more memorable. This stands for Danger, Response, Send, Airway, Breathing, CPR, Defibrillation, each of which is a key step in the resuscitation process.
But a general rule, the medical community recommends that if you come across someone who is both unconscious and lacking a pulse, you should always assume they’re suffering cardiac arrest. Statistically speaking, this saves the largest amount of lives. When that’s the case, your first step is calling 000 for assistance. The second is to commence CPR – prolonging the person’s life as long as possible. After this, the next step is defibrillation.
As a general rule, if more than one person is present to help when a person is suffering cardiac arrest, one person should commence CPR as soon as possible while others call 000 and seek out an AED. Both play a critical role in resuscitation. Without CPR providing oxygen to the person’s brain, they could be dead in minutes. But the odds of CPR alone reviving a cardiac arrest victim are very low – you’ll need additional help and very likely defibrillation to have much chance of reviving them.
Of course, all of this is covered in CPR training.
It’s worth knowing, most countries nowadays – including Australia – have what’s called good samaritan laws. Effectively this means if you’re genuinely trying to help in an emergency, you can’t be sued or prosecuted for making a genuine mistake (unless you’re intoxicated or behaving in a clearly reckless manner). Combined with the fact that AEDs take a lot of the tough choices out of your hands, this means that you don’t need to worry about getting in legal trouble for trying to help in an emergency. So there’s no reason to hold back on hooking a casualty up to an AED.
How To Use A Defibrillator?
Generally, an AED is the only sort of defibrillator a non-medical professional should attempt to use. The other types are either highly technical pieces of equipment that only medical personnel should have access to, or are wearable (or surgically implanted) devices that operate automatically and take care of themselves.
AEDs are designed to be as intuitive and easy to use as possible – they’re designed to be used by non-experts in a crisis. There are many AEDs on the market, and they don’t all look or operate the same, but generally, the instructions (written or spoken by recorded voice) should make it quite clear how to operate the device.
Defibrillator Sign / AED Sign

AEDs have become a common piece of first aid equipment in public venues in recent years. While the public symbols for first aid are widely known, AEDs are now common enough to need their own symbol – something that could be easily and quickly recognised in a crisis. The current standard is a white heart on a green background with lightning through the middle of the heart and a small cross in the upper right. This is now well recognised in many countries, including Australia.
In some places, the heart might be red or white on a red background (harkening back to the colours of the Red Cross), and the cross may be absent. But generally, if you see the image of a heart with a lightning bolt across it, it’s usually pointing you to an AED.
Defibrillator Pad Placement
AEDs will generally come with detailed instructions for placing the pads, but as a general rule, you’re aiming for the electrical current from the pads to flow through the region of the heart. One pad is normally placed on the right upper chest – above the right nipple and with the top of the pad on the collarbone. The other pad should be on the ribcage under the left breast, curving around the chest so it’s partly under the arm.
If you imagine a clock in the centre of the person’s chest with hands showing 10:20, the hands will point to the ideal location of the pads.
Be Ready For The Worst Case Scenario
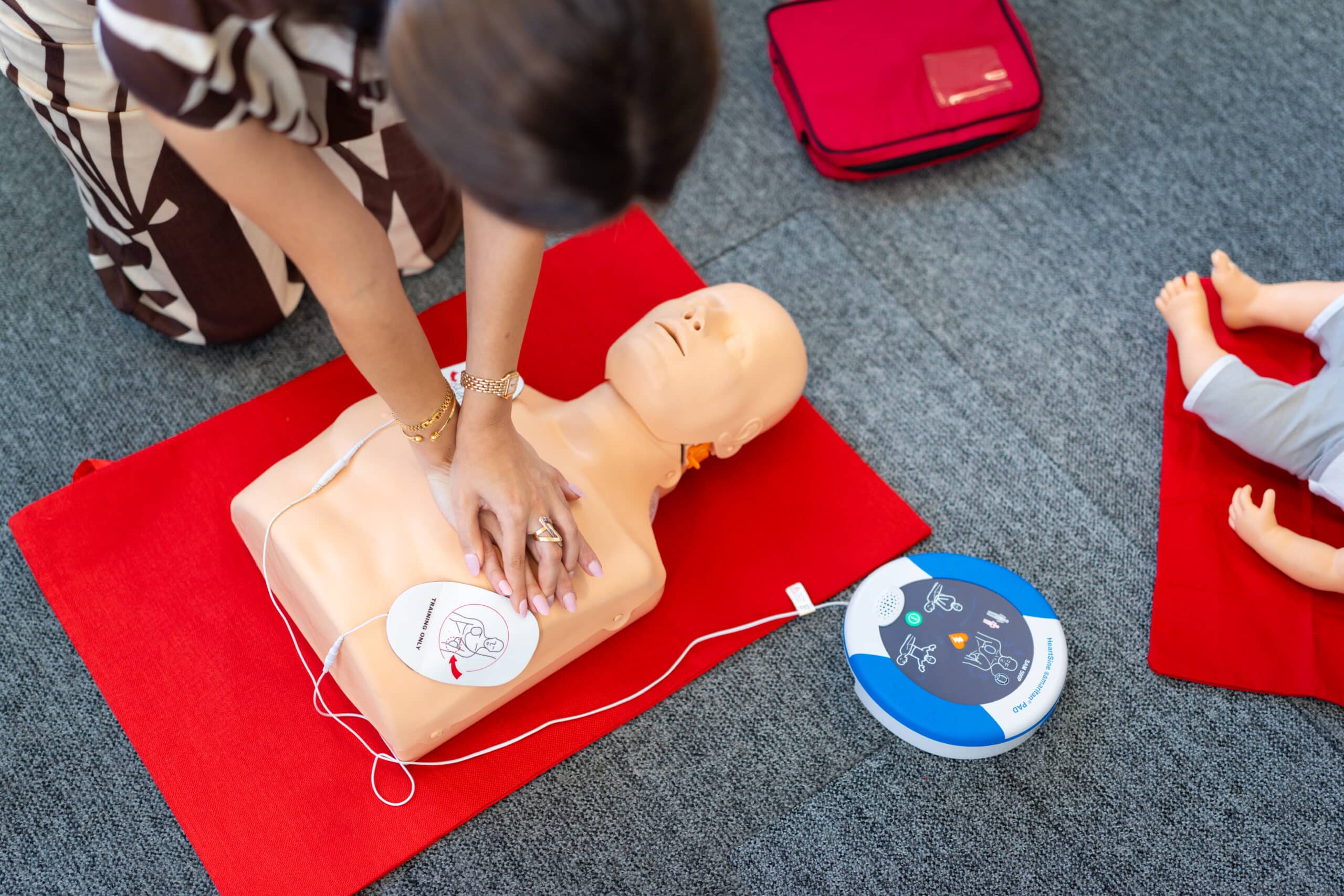
It only takes around 2 hours to complete a fully certified CPR course, and it costs less than filling up your car. For many people, this is simply a professional requirement for a role, but courses are also open to members of the general public. The training covers the fundamentals of CPR and the use of an AED – including the chance to try out a practice unit. If you’re keen to know how to help someone suffering a cardiac arrest – and potentially save a life – it’s one of the best investments of time and money you could make.